
Take Towcester Vets’ safety quiz for preventing dog bites
Dog bite prevention week is recognised in many countries between April & May each year to bring attention to the risk of dog bites and share preventative advice. In this article, the team from Towcester Vets are sharing important tips and resources to help Towcester residents prevent dog bites in children and adults.
April 1st – May 2nd is also National Pet Month, in which responsible pet ownership is the theme and a perfect backdrop for this article’s topic.
13 tips for preventing dog bites
Most dog bites don’t come from dogs who are deemed ‘aggressive’, they occur in the home with family dogs or dogs who are well known. Pets who are described by their owners as placid, loving, and “wouldn’t hurt a fly” can all snap and bite if they feel agitated, threatened, frightened, vulnerable, unwell, or in pain.
As well as the obvious physical injury, a dog bite can cause complex psychological issues. If a dog bites a child (or lunges at them) especially, they can develop a long-term fear of all dogs. Dogs can ‘learn’ that this behaviour is needed to stop the action that is bothering them. This is a real shame as children and dogs can both benefit from forming a close bond together.
Therefore, it is advisable to practice these 13 do’s & don’ts of dog interactions:
- Do choose the right dog breed for your family and home setup – remember, all cute puppies grow into adult dogs with big teeth
- Do ensure your puppy’s (or older dog’s if you missed this stage) socialisation experiences include being around children
- Do train your pet from a puppy into adulthood on how to be well-mannered in the home and out & about
- Don’t use fear to train a dog as this is harmful and can lead to unwanted reactions in everyday situations
- Don’t assume your dog won’t bite just because you perceive it not to be in their nature
- Don’t leave children alone with dogs
- Do teach children from a young age how to behave around dogs, including not playing aggressive games with them, pulling their ears or tail, or anything else that may agitate them
- Do act calm around dogs, especially if they are unfamiliar to you
- Do supervise children feeding or walking a dog
- Don’t let your child discipline a dog
- Don’t invade a dog’s space without their permission – let them come to you (avoid letting young children hug & kiss dogs)
- Do teach children to always ask the owner’s permission to stroke their dog and where the dog likes to be stroked
- Don’t allow your child to approach a dog in someone else’s garden or car
Socialisation & training
Puppy socialisation begins not long after birth, when they will learn how to be a puppy from their mother and siblings. When puppies go to live with their new owners (typically from 8 weeks old), there is a key window up to 12 weeks of age, during which puppies should undergo more practical socialisation with their new owners. Your puppy’s brain will be like a sponge at this age, absorbing all the sights, sounds, smells, tastes, experiences, and opportunities to learn that they can. Most older dogs can be socialised too, however it may take a lot more time and patience.
An excellent resource for puppy socialisation is The Puppy Plan from Dogs Trust
Socialisation and training (into adulthood) are not about obedience. They are about building confidence and developing clear communication with your dog. If your dog understands your request and how to respond to it and has self-confidence, they are less likely to get fearful or frustrated, which are both common causes of dog bites.
Ask our Towcester nurses for puppy socialisation advice on our Facebook page here
Learn how to be safe around dogs
The team from Towcester Vets recommend these helpful resources below to help your whole family become smarter and safer around dogs.
First, take our Dog Safety Quiz to test how much your family members currently know.
Then, work through these Dogs Trust resources and get everyone to re-take our Quiz.
Remember, don’t give the answers away until after retaking the quiz!
Let us know how you got on by sharing your results on our Facebook page.

Calf Scours – Prevention is Possible!
Scouring calves can be frustrating but prevention is possible through good hygiene, colostrum management and an understanding of the causes of disease on your farm.
1. Good hygiene
- Good hygiene is essential for preventing the build up of infectious pathogens
- Regularly muck out and disinfect calving pens
- Dip navels in iodine immediately after birth and again 4 hours later
- Isolate any sick calves and clean out areas that have been contaminated
2. Colostrum management
- Colostrum gives calves antibodies to help protect them from disease
- Ensure colostrum is of good quality
- Consider metabolic profiling cows 2-3 weeks before calving to ensure they are in optimum condition to produce high quality colostrum
- A refractometer can be used on farm to assess colostrum quality
- Ensure calves receive the right quantity of colostrum, quickly enough
- Calves should receive 3l of colostrum within 2 hours of birth, and a further 3l within 24 hours
- Blood samples can be taken from calves within the first week of life to assess colostrum uptake
3. Quick and effective treatment
- Isolate scouring calves away from other calves and clean any contaminated areas to prevent spread to other calves
- Give supportive care
- Keep calves warm and dry; consider using calf jackets
- Keep calves hydrated with oral fluid therapy
- Give 1-2l of electrolytes 4 times daily
- Alternate with milk every 4 hours
- Diagnose the cause to inform treatment
- Take a temperature
- Normal temperature should be 38.0 – 39.5°C
- A high temperature indicates a systemic bacterial infection
- A low temperature may occur with severe dehydration
- Consider the age of the calf since different causes are associated with different ages of calf:
- Take a temperature
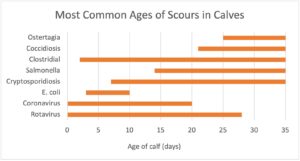
-
-
- Use an on farm calf scour test kit to diagnose E. coli, Coronavirus, Rotavirus and Cryptosporidiosis
- Submit a faecal sample
- We can look at faecal samples in house for coccidia and worm eggs, and carry out a scour test if you haven’t got one on farm
- We can send faecal samples to the lab to test for Salmonella, E. coli, Cryptosporidiosis, Rotavirus, Coronavirus, Coccidiosis and worms
- Treat appropriately
- Antibiotics
- Injectable antibiotics are essential for treating bacterial infections including E. coli and Salmonella, indicated by a high temperature
- It is also beneficial to treat calves with antibiotics even if they are infected with viruses or parasites, since they are at higher risk of bacterial infection
- Anti-inflammatory pain relief
- Meloxicam (Animeloxan/Meloxidyl) reduces inflammation and pain associated with intestinal disease
- Specific treatments
- Cryptosporidiosis can be treated with halofuginone lactate (Halocur)
- Coccidiosis can be treated with Baycox or Vecoxan
- Ostertagia can be treated with most wormers
- Other drugs
- Steroids or anti-spasmodics may be helpful in severe cases of diarrhoea – talk to a vet about whether these are appropriate
- Antibiotics
-
4. Specific preventative measures
- Use diagnosis to inform your prevention strategies
- Cows can be vaccinated for rotavirus, coronavirus and E. coli so antibodies pass to calves in colostrum
- Pasture management is important in controlling coccidiosis and worms
- Talk to a vet about how to tailor a calf scour prevention strategy to your farm


Identifying & Preventing Staggers in Cattle & Sheep
Staggers is caused by low blood concentration of magnesium and affects both sheep and cattle. It is most commonly seen in adult lactating animals grazing lush, fast-growing grass pasture but we do see a number of cases in housed animals every year. Magnesium isn’t stored in the body and therefore the main source is from food. Absorption will vary with how quickly food passes through the digestive tract and there will be a higher demand during lactation. If feed intakes are reduced due to stress, illness or poor weather then this will also affect magnesium absorption.
Magnesium is important in normal neurological function. Clinical signs therefore include:
- Sudden death
- Initial excitability with high head carriage, twitching of muscles and incoordination.
- Separation from the group. Animals may have startled expressions, exaggerated blink reflex and frequent tooth grinding.
- Rapid progression to periods of seizure activity
Animals found with clinical signs require immediate treatment with subcutaneous Magniject whilst waiting for veterinary attention to administer a combination of calcium and magnesium slowly into the vein. Stress should be minimised during this time and unfortunately there is always a risk during treatment that the extra stress could kill the animal. If treatment is successful, animals should be offered concentrates and good forage to prevent relapse.
In cases of sudden death, we can confirm the diagnosis by measuring magnesium concentration in the fluid around the eye soon after death. Blood sampling a few other animals in the group can also be useful as the majority of the group may be affected without showing obvious clinical signs.
Factors influencing the availability of dietary magnesium include magnesium levels in the soil and grass which vary considerably. High levels of potassium or ammonia on pasture inhibit magnesium absorption. Lush pastures are low in fibre and increase the rate of passage of food material through the rumen reducing time for magnesium absorption.
In terms of prevention, options include:
- Medicating the sole water supply with soluble magnesium salts such as chloride, sulphate or acetate. These salts aren’t very palatable so follow directions for use carefully.
- Intra-ruminal boluses which give a reliable slow release of magnesium into the rumen over periods of high risk.
- Magnesium buckets though these may not be used by all animals in a group and problems can still occur.
- Supplementation is particularly important during stormy weather when roughage, such as straw, can be beneficial by slowing rumen throughput and allowing time for magnesium absorption.
- Feeding concentrates containing magnesium will also help to provide sufficient amounts.

Newborn Cria Care
Summer is an exciting time for new arrivals! Whilst most camelids manage this period without any problems, by keeping a close eye on newborns, any problems can be spotted and treated early ensuring happy, healthy babies.
Vaccination
Most herds will booster vaccinate pregnant females in the run up to unpacking (between 2 and 8 weeks prior). This aims to boost the level of antibodies in the colostrum conferring protection to the cria. Crias can then be vaccinated around 3 months old with a full primary course.
Newborn care
Newborn crias should be standing within the first 30-60 minutes and nursing within 2-4 hours. Mum should also pass her placenta within 2-4 hours of birth. Navels should be dipped in iodine tincture to help to dry it and to reduce the risk of infection via this route. If crias aren’t nursing within this time frame then they may need help to suckle or try to milk the mum (we appreciate this isn’t very easy!) and feed this to the cria by bottle. Any cria that is struggling should be checked carefully for potential problems such as a cleft palate. Hernias are also quite common so check the umbilical region carefully. Monitor crias to ensure they pass their first poo within 24-36 hours.
Failure of passive transfer (FPT)
Crias are born with no antibodies, making them extremely susceptible to infection. Young camelids get the important antibodies from the colostrum of their dam so ensuring they get their first drink is really important to protect them from infections. Crias should consume 10-20% of their body weight in the first 24 hours of life (equating to 700-1400ml for a 7kg cria).
Crias can fail to absorb antibodies for a variety of reasons but certain situations put them at higher risk. If any of the situations on the list below apply, then we recommend checking your new arrival for failure to absorb enough antibodies, called Failure of Passive Transfer (FPT).
- Low birth weight (<6KG in alpacas and <7kg in llamas )
- Evidence of prematurity (curled ears, unerupted incisors, socks on feet)
- Difficult birthing or caesarean
- Congenital defects (e.g. cleft palate)
- Maternal issues (first time mum, no bond between mum and baby, no milk, mastitis)
Crias should be weighed daily during the first few weeks of life to and crias that aren’t thriving or aren’t putting on weight should also be assessed. They should generally gain 0.1-0.45kg daily.
Crias with FPT are at risk of life threatening infections so it’s important we check early enough that we can correct the problem before this happens. We recommend checking when the cria is around 24-48 hrs old. The check is a quick and easy blood test that can be performed at the surgery. Crias who are shown not to have enough antibodies can then receive a plasma transfusion to boost antibody levels before infections can set in. If your herd does not currently have any plasma available then do let us know and register your interest for our next Blood Drive Day (2023)
Feeding crias
If mum doesn’t have enough milk then supplementation with other products will be needed. In the first 24 hours, colostrum is vitally important. If camelid colostrum can’t be sourced (this may be unlikely!) then goat’s colostrum is the closest alternative, followed by cow colostrum. If sourcing colostrum from a farm, do be aware of the risks of TB, Johne’s and BVD and only source from herds free of these diseases. Powdered colostrum supplements are available but they generally contain very few antibodies in comparison to camelid colostrum so crias who receive these are at much higher risk of FPT. The product with the highest amount of antibodies is called Immucol Platinum and can be sourced via the Camelid Veterinary Services online shop.
If bottle feeding, aim to feed 10-15% of bodyweight over 24 hours split into 2 hourly feeds initially. Crias feed little and often so this aims to replicate this behaviour. Overfeeding can result in milk entering the wrong stomach and can lead to problems. After 24 hours, milk can be used for feeding as crias are no longer able to absorb colostrum, goat’s milk is the closest alternative to camelid milk.

Towcester Vets offer tips on how to be a responsible cat owner
National Pet Month (April 1st – May 2nd) promotes responsible pet ownership, but what does that mean when it comes to cats? Many people believe that cats “pretty much take care of themselves”, and their aloof behaviour means they have little interest in or need for their human companions. Our helpful Vets here in Towcester are here to tell you why this is not the case.
Cats actually become very attached to their humans. Like dogs, cats can suffer from separation anxiety too, although they’re usually not quite as vocal and destructive about it.
At Towcester Vets we believe that being a responsible pet owner means ensuring your cat has everything they need to live a healthy, happy, and fulfilled life. To help you, the cat-loving Vets at Towcester have pulled together the ultimate cat care list for you.
Cat care 101 – How to take care of a cat
1. Provide calm & comfort – Cat care starts with a comfortable home environment that’s as stress-free as possible – remember not all dogs and cats, or multiple cats will get on. A plug-in pheromone diffuser can help to ease tensions between pets.
2. Get these essential items – There are many options when it comes to cat beds, including those that hang over radiators, and yours of course! Your cat might prefer a certain type or a combination. They will also need litter trays, and food & water bowls. Multiple cat households need a litter tray per cat, ideally on each level of your house, and separate food & water bowls away from the litter trays. If your cat likes to roam, fitting a microchip cat flap will give them the freedom they desire.
3. Commit to lifetime cat vaccinations – Making sure your cat is vaccinated every year will help to protect them from harmful and life-threatening contagious diseases, keeping them healthier for longer.
4. Take your cat for regular health checks – Your cat will receive a thorough health check at their annual cat vaccinations appointment at Towcester Vets. Having 6-month checks-ups in between their boosters can help our Vets to spot any health issues early.
5. Keep up to date with parasite control – The best way to avoid your cat picking up fleas or worms is to give them vet-recommended cat flea & worm treatments regularly. These are typically given monthly and help to protect your pet from the nasty effects of parasites.
6. Get your cat microchipped – A press release was published on the UK Government website recently stating that microchipping cats is going to become mandatory with fines for non-compliance. Get ahead of this new law and get your cat microchipped, which most importantly increases your chances of being reunited with them if they go missing.
7. Give your cat a nutritious diet – Hard kibble is important for dental health, wet food provides moisture, avoid human foods, and opt for good quality food brands. Our Vets & Nurses can provide you with more in-depth, expert advice tailored to your cat’s life-stage, activity level, and current health. Chatting to us before changing cat foods is wise too as even small changes can have a big impact on your cat’s health.
8. Try these cat enrichment ideas – Boredom and loneliness can affect your cat’s behaviour and health. Avoid this by spending plenty of time with your cat playing, grooming, or simply snuggling up together, and by providing cat enrichment toys and activities. Our team of friendly Vets recommend scratching posts and searching YouTube for how to build a cat home gym.
9. Get a cat sitter for holidays – Booking a cat sitter at your home (or taking them to a cattery if this is not possible) will ensure your cat still gets everything they need when you’re away, bar you.
Now, we don’t want you to think that all cats are high maintenance after reading this (well, some are), but we should point out that owning any pet is a big responsibility. If you have any concerns about your cat’s health, come and see one of our Vets in Towcester.

SCOPS Nematodirus Forecast, Risk factors, Action & Treatment
The SCOPS Nematodirus forecast predicts the hatch date for Nematodirus based on temperature data from 140 weather stations throughout the UK.
At Towcester Farm Vets we monitor the three weather stations in our area and put a notification on our Facebook Page if the forecast status in our area changes. The stations we monitor are Church Lawford, Bedford & Woburn. If you follow us on Facebook we’ll let you know as soon as one of those stations indicates a change in its status.
The information below is based on the material on the SCOPS website and is designed to be used in combination with your grazing history (more below) to assess the risk of your lambs becoming infected.
Using the SCOPS forecast
- Use the SCOPS map to locate the station(s) closest to your holding.Use knowledge of your farm and the surrounding area to choose a weather station that is most relevant to you. In most cases this will be the nearest station but if, for example, there is a large difference in the height above sea level between your holding and the nearest weather station, then look to see if another station further away may be more representative. If you click on a station on the SCOPS map, it will give the height above sea level. Alternatively take a view across a combination of stations in your area.
- Click on the station(s). Each station has more detailed information on the current risk level, guidance on what to do next, and information on when the forecast was last updated.
- Carry out a risk assessment and take action if needed. See below for more information on how to assess risk and what action to take.
- Consider additional information to the forecast map.
- The map predicts hatch date on temperature data, but the risk will vary from farm-to-farm and from field-to-field. When deciding whether or not to act, it is important to assess the risk to each group of lambs based on the history of the field, its aspect and altitude.
- South-facing fields tend to have an earlier hatch and, as a guide, every 100m increase in altitude will delay hatching by about seven days. So, for example, if your nearest weather station on the map is at 200m above sea level and your farm is 100m above sea level, hatching could be around seven days earlier than the forecast.
- You can also click here to see a table capturing data from the map over the previous weeks, so you can see when the dot indicating your nearest weather station changed colour. You will need to know the name of your nearest station to find it in the table, so click on that station on the map above to check the name.
Understanding Nematodirus
Nematodirus is a particularly nasty disease in lambs, causing a high number of mortalities and stunting the growth of many others. It is caused by the Nematodirus battus worm, which has a different lifecycle to other sheep worms. Under certain climatic conditions it can strike very quickly, with little or no warning. The main difference in the lifecycle of Nematodirus battus compared with other parasitic worms is that development to infective larvae takes place within the egg and infection passes from one lamb crop to the next year’s crop. Cold weather delays hatching so when we get a sudden change in temperature it can trigger a mass hatch. If this coincides with the time when lambs are starting to take in significant amounts of grass (over about six weeks old), the result can be devastating.
Nematodirus can strike very quickly so you can’t afford to have a ‘wait and see’ policy. And because the damage is done by large numbers of immature larvae that are not producing eggs, faecal egg counts (FECs) are not a reliable indicator of risk. Rapid action is often required and this has to be based on a risk assessment and the forecast for your area.
Main risk factors
If your lambs are grazing pasture that carried lambs last spring and you answer yes to one or more of the four questions below, then your lambs are at risk.
- Are your lambs old enough to be eating significant amounts of grass? (generally 6-12 weeks of age but may be younger if ewes are not milking well)
- Do you have groups where there is also likely to be a challenge from coccidiosis? For example, mixed aged lambs are a higher risk
- Has there been a sudden, cold snap recently followed by a period of warm weather?
- Have you got lambs that are under other stresses e.g. triplets, fostered, on young or older ewes
Recommended actions
- If possible, avoid infection. Move at-risk lambs (as determined by the risk assessment) to low risk pastures (i.e. pasture that was notgrazed by lambs the previous spring).
- If you cannot avoid high risk pasture grazed by lambs the previous spring and decide you need to treat for Nematodirus, SCOPS advises farmers to use a white (1-BZ) drench. Check that treatment is effective by taking a FEC 7 to 10 days after treatment. Remember, it may be necessary to treat lambs more than once depending on the spread of ages in a group and subsequent weather conditions.
The timing of a potential problem will vary from region to region. In the south of England for example, it is likely to occur earlier in April/May; in northern England and Scotland it may be early June.
Treatment
As explained above, SCOPS advises farmers to use a white (1-BZ) drench when treating. These are normally highly effective against this parasite and suitable for young lambs. However, the first confirmed case of Nematodirus resistant to the 1-BZ group was reported in 2011 and so farmers are advised to follow the SCOPS guidelines on correct drenching technique and dose carefully to the correct weight of the lambs and to check afterward if the treatment has been fully effective. If in doubt speak to one of our vets by calling us on 01327 350239.

Cats, dogs and bee stings – what you need to know
Cats and dogs are naturally inquisitive animals. This has many benefits but can also get them into trouble! A common problem in the spring and summer months is Bee or Wasp stings. Our Veterinary Nurses have some advice for Northamptonshire owners of cats and dogs on this topic.
To help you tell the difference between bees, wasps, and hornets, our team have put together a handy guide for you to download.
Why do bees sting cats and dogs?
Often in the warmer months we spend more time outdoors and naturally our animals will then spend more time nosing at the flowers. This is typically how cats and dogs get stung as their inquisitive noses disturb the bees and wasps collecting pollen. Trying to catch a buzzing insect can also seem like a fun game…until they get stung!
Signs that your cat or dog has been stung
In most cases, owners will not actually see the stinging occur. Instead, you may see your pet suddenly shaking or pawing at their head or body, or they have a swollen face all of a sudden.
Typical bee and wasp sting symptoms include:
- Swelling (often around the muzzle where they have been sticking their nose in)
- Constantly licking either at a specific area or their lips if the sting is inside the mouth
- Redness around the area where the sting went in
- Pawing at the area
- Sneezing
- Vocalising more than usual
Severe symptoms could include:
- Brachycephalic breeds can have added breathing difficulties if the sting is around the throat area
- Vomiting and diarrhoea
- Allergic reaction such as anaphylactic shock (although this would be very rare)
How to treat a bee or wasp sting on a cat or dog
Unless you saw the stinging occur, it will be difficult to tell if your pet was stung by a wasp or a bee. Either way, you can use our first aid tips below.
First, you want to make sure the sting is removed. Our Towcester Vet Nurses suggest using something flat like a credit card to scrape the sting off your pet’s skin and dispose of it. Avoid using tweezers to pull the sting out as they could squeeze venom into your pet.
Second, if you do know whether it was a bee or a wasp, you could apply the correct substance to soothe the pain;
- Wasp = vinegar/lemon juice
- Bee = bicarbonate of soda & water paste
Do you know the difference between a bee and a wasp? Download our Know Your Insects Guide
If you do not know the culprit, or after you have used the above first aid advice, you can then apply a cold pack to the swelling.
When to call a Vet
If you are at all concerned, especially if the swelling is causing further distress to your pet or is likely to affect an airway, you should always ring a Vet for advice. Our Burcote Road veterinary team are here to help, just give us a call on 01327 350239.
Some pets may need pain medication, which can be prescribed by one of our Vets too.
Northamptonshire pet owners sometimes ask if they can use antihistamines to help with the reaction; these can only be prescribed by the Vet to ensure the correct dosage is given, and because some ingredients could possibly be fatal in some brands.
Just to be safe this season, why not print our Know Your Insect guide and stick it on your fridge to help you spot the differences between bees, wasps, and hornets?
Remember to share this advice with your pet-loving friends on Facebook!

Understanding laminitis in horses & ponies
Veterinary Surgeon Holly Gimmler has written this short article looking into the causes, diagnosis and treatment of laminitis as well as the implications for ongoing management once a horse has suffered from this common condition.
What is laminitis?
Lamellae are the soft tissue structures that hold the pedal bone in the foot to the hoof wall. Laminitis occurs when these tissue structures become inflamed. It’s a common and painful condition which often results in lameness. Laminitis normally affects both front feet, but it can affect all feet.
What causes laminitis?
Although often considered a disease of overweight ponies, laminitis can be triggered by a variety of metabolic or physical causes in any horse, including:
- Endocrine disease e.g., Equine Cushing’s (pituitary pars intermedia dysfunction; PPID) and equine metabolic syndrome (EMS)
- Diseases causing inflammation, such as colitis
- Mechanical overload such as supporting limb laminitis
- Concussive laminitis from trauma to the feet
There are many predisposing factors, including obesity and seasonality. Spring and Autumn are the times of highest risk for laminitis as the sugar content in grass peaks. However, laminitis can present itself at any time of the year.
How do I know if my horse or pony has laminitis?
Common clinical signs include:
- Lameness
- Reluctance to move, or short pottery steps
- Preferring soft surfaces to hard or stony surfaces
- Difficulty turning in tight circles
- Unwilling to pick up feet
- A “rocking” stance, or weight shifting backwards or between feet
If your horse or pony exhibits any of these signs, it is important to call a vet.
Your vet will examine the patient to rule out other causes of lameness, or other conditions that can present similarly (colic, foot abscess, tying up). Your vet may also identify strong and bounding digital pulses, sensitivity on application of hoof testers and an elevated heart rate or sweating and distress.
Treatment in the first instance
- Box rest on deep shavings as this helps to pack the foot, providing support
- Pain relief, as prescribed by your vet. The first line option is often phenylbutazone (bute), sometimes in conjunction with paracetamol
- Your vet may recommend taking a blood sample to diagnose underlying diseases which can then be addressed or managed
- In severe cases there can be sinking or rotation of the pedal bone. Your vet may take x-rays of the feet to assess the severity of this
- Sadly, in severe cases where the pain cannot be controlled, euthanasia is recommended to relieve the horse of suffering
Ongoing management of laminitis
Unfortunately, once a horse has had laminitis it is more likely to suffer in the future. Good ongoing management therefore becomes very important.
- Dietary restriction. Aim for 1.5% bodyweight hay per day, ideally soaked. Hay need only be soaked long enough to leach out the soluble carbohydrates (sugars), so 30-45minutes at most. Avoid concentrates as these are rich in carbohydrate. Strip grazing or grazing muzzles should be considered for particularly good do-ers during high-risk periods
- Arrange a farrier visit to help address discomfort and stabilise the feet; there are specific shoes that may be recommended to provide support
- Schedule frequent reassessments with your vet to monitor your horse or pony’s comfort and progress
Holly Gimmler BVSc MRCVS
Holly joined our equine veterinary team in July 2021 having just graduated from the University of Liverpool. During her studies she gained valuable experience treating equine emergencies and caring for inpatients under the guidance of top specialists at the Philip Leverhulme Equine Hospital. She enjoys all aspects of equine veterinary work and has gained particular interests in anaesthesia, medicine and reproduction.

Cat hay fever symptoms & treatments you need to know about
So, can cats have hay fever?
It is one of the most common illnesses in cats, yet many Northamptonshire owners are not aware of it. Hay fever, at its worst during spring and summer, does in fact plague both humans and animals alike.
At Towcester Veterinary Centre, we have seen many cats with a grass or tree pollen allergy. It affects the skin more than it does the sinuses and can make your pet chronically ill. Fortunately, there are things you can do to help…
1. Be aware of cat hay fever symptoms
Excessive licking and scratching are signs that are often associated with fleas, but they can also be brought on by an allergic reaction to pollen. This can make the skin, ears, and bottom very irritable and itchy. Plus, if your cat has bald patches around the lower back, groin, tail, or paws, there is a high chance they are suffering from hay fever.
2. Check for fleas
So that you do not confuse hay fever with fleas, Towcester Veterinary Centre’s nurses recommend that you should check your pet’s fur for flea dirt. You should also ensure your cat is up to date with their preventative parasite treatments. Most spot-on pipettes and tablets need to be given monthly.
3. Treatment of cat hay fever
If you are concerned your cat may have an allergy, bring them in to see one of our Vets. We can run tests to help pinpoint the problem and, if needed, subscribe treatments such as antihistamines and anti-allergy vaccines.
Important: Never give your cat human medicines unless instructed by your Vet as only some are safe for cats and dosages will differ.
4. Preventative measures?
It is hard to avoid pollens, as many hay fever sufferers in Northamptonshire will know. Sometimes even staying indoors to avoid pollens can still be miserable and forcing your cat to stay in can damage their health in other ways. In addition to anti-allergy injections or antihistamines, here are some other ways to help your cat beat hay fever:
- Evening primrose oil can be effective in reducing a reaction – drop into your cat’s food or directly into their mouth, or on their nose to lick off
- Wash your hands before and after handling your cat to reduce the transference of pollen
- Wipe your cat’s fur when they come inside with a damp (but not soaking) cloth to remove some of the pollen
- If your cat is willing, an occasional bath can help to remove pollen from their fur
We are here for you and your pets, so do get in touch if you would like more advice on cat hay fever.

Towcester Vets share spring safety tips for dog, cat & rabbit owners
Dogs, cats, and rabbits have many differences, which is why we choose them as pets. However, as the spring season gets underway and the flowers start to bloom, these three species have a few things in common… The team at Towcester Vets are sharing advice on common dangers that can affect all pets this season.
To help owners of dogs, cats, and rabbits further, Towcester Vets’ nurses have pulled together some extra tips for keeping pets happy and safe in spring – download these below.
Download our Spring Safety Tips
Be aware of these common spring dangers
Parasites on & in pets
Dogs and cats are prone to catching fleas if they are not regularly treated with vet-recommended parasite prevention products – ask us about these. Fleas can be difficult to get rid of as they lay eggs and multiply extremely quickly, living in your carpets and furniture as well as on your pets. Worms can be problematic too if your pet isn’t treated regularly. Lungworm in dogs can be fatal – get tips about this and other spring safety advice here >
Rabbits can get fleas and worms too, but they are mostly a target for flies. Flystrike in rabbits occurs when blowflies (green & blue bottle) lay their eggs on or near a rabbit’s anus, after being attracted by faeces and urine. The hatched maggots then feed on the rabbit’s flesh. Flystrike is a painful and life-threatening condition. A clean and dry rabbit and hutch will be less appealing to flies.
Pet diseases
Parvovirus, Distemper, Feline Leukaemia, Cat Flu, Myxomatosis, and Viral Haemorrhagic Disease (VHD) – these are just some of the life-threatening contagious diseases that pets are at risk of. All of these diseases are preventable through annual vaccination.
Our experienced team of Vets advise that vaccinating your pet not only protects them, but protects other pets too by reducing the spread of disease. Parvovirus and VHD can be carried on inanimate objects including shoes, car tyres, clothing, and food bowls.
Pet poisons
Common spring pet poisons can be found in many homes and gardens in Towcester. Spring is synonymous with spring cleaning, indoors and out, and this can mean many toxic substances being left where pets can access them. Keep products out of reach and behind closed doors when they are not in use.
Many garden and house plants are poisonous too – do a search online for ‘poisonous plants for rabbits’ or ‘plants that are toxic to dogs’, or cats. Do you have any of these? Common culprits are lilies, foxgloves, rhubarb, daffodils (bulbs especially), and tulips. For the safety of your pets, our Vets recommend removing them or putting in measures to ensure your pets cannot reach them.
Now to an extremely common poison this time of year – chocolate! With Easter on the horizon, there is likely to be more chocolate in your home than usual. Chocolate is extremely toxic to all pets and should always be kept well out of reach. If you think your pet could have eaten any, contact us straight away on 01327 350239.
We hope you found our information on springtime dangers useful. Get our extra Spring Safety Tips for dogs, cats and rabbits here:

